|
Repair of congenital pulmonary vein stenosis
Ying-Long Liu, Xiang-Dong Shen and Jian-Rong Li
Beijing, China
Author Affiliations: Fuwai Cardiovascular Disease Hospital, Chinese Academy of Medical Sciences & Peking Union Medical College, Beijing 100037, China (Liu YL, Shen XD and Li JR)
Corresponding Author: Jian-Rong Li, MD, Laboratory of Congenital Heart Disease, Fuwai Cardiovascular Disease Hospital, Beijing 100037, China (Tel: 86-13811398232; Email: leejianrong@126.com)
Congenital pulmonary vein stenosis (CPVS) is a rare fatal congenital cardiovascular defect and its operative mortality is very high. A 6-year-old boy presented with bilateral congenital pulmonary vein stenosis complicated by severe pulmonary hypertension and mitral in-sufficiency. A successful angioplasty in combination with mitral valvuloplasty was performed for pulmonary veins with living autologous atrial tissue and sutureless in situ pericardium.
Key words: pulmonary vein stenosis; congenital heart disease; surgery
World J Pediatr 2006;4:308-310
Introduction
Congenital pulmonary vein stenosis (CPVS) is a rare malformation with a high mortality, and no successful treatment of this disease was reported in China. We report a child with bilateral CPVS complicated by severe pulmonary hypertension and mitral insufficiency, who underwent a successful angioplasty for pulmonary veins with living autologous atrial tissue and sutureless in situ pericardium in combination with mitral valvuloplasty at our pediatric center of cardiovascular surgery.
Case report
A 6-year-old boy felt fatigue, palpitation and dyspnea on exertion in recent 6 months and had lost consciousness while playing games repeatedly in the last 4 months. No characteristic manifestations but pulmonary hypertension were found on physical examination, electrocardiogram and chest film. Findings of echocardiography with color Doppler examination helped to diagnose his disease as CPVS complicated by pulmonary hypertension and mitral insufficiency. Stenosis of the junctional areas was observed between the 4 pulmonary veins and the left atrium. The diameter of the pulmonary veins was about 4 mm with a venous flow velocity of 2.2 m/s, and a tricuspid valve regurgitation jet with a velocity of 4.7 m/s (i.e., an estimated right ventricular pressure of 95 mmHg), and moderate mitral regurgitation was noted. Further investigation of ultra fast computed tomography (UFCT) confirmed the diagnosis (Fig.).
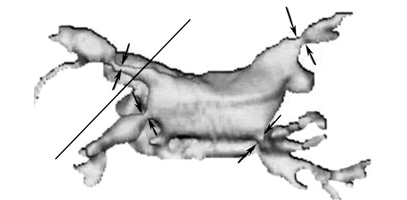
Fig. UFCT 3D computer-generated picture of narrowed pulmonary veins. Arrows: the areas of stenosis.
Operation was performed on June 1, 2005. The pulmonary artery was infused with 4ºC protective solution during cardiopulmonary bypass (CPB). After the interatrial septum was incised, the left atrium and mitral valve were explored to probe the orifices and adjacent extrapulmonary venous segments of the pulmonary veins were probed. There were severe tubiform stenosis in the orifices of the left superior, left inferior and right inferior pulmonary veins and membranous stenosis in the extrapulmonary segment of the left superior pulmonary veins, which was about 2 cm away from the orifice, without any abnormality in the vessel wall. Anular dilatation was the main cause of mitral regurgitation. The apex of the heart was retracted anteriorly and rightward to expose the left atrial appendage and the left pulmonary veins. A V-shaped incision was made with one limb through the anterior wall of the left superior pulmonary vein and the other through the left inferior vein. The tip of the left atrial appendage was opened by a fish-mouth incision and sutured to widen the opening in the pulmonary veins. This provided a double pathway for left pulmonary venous return. The stenotic membrane of the left superior pulmonary vein was excised. The right inferior pulmonary vein was incised from its ostium, all the way up to the pericardial reflection, to reach normal segment. Then a flap of the native pericardium was anastomosed to the right atrial wall to create a pouch of the in situ pericardium that passively drains the right inferior pulmonary vein into the wide-open left atrium. The dilated annulus was repaired by anuloplasty. Postrepair cardiac function was good, and after discontinuation of the cardiopulmonary bypass, the mean pulmonary arterial pressure was 34 mmHg (52 mmHg before operation).
The postoperative course was uneventful and echocardiography showed that the stenosis in the pulmonary veins disappeared and the venous flow velocity was normal. The patient was discharged from the hospital 7 days after the operation.
Discussion
CPVS, a rare fatal congenital cardiovascular defect with a very high operative mortality, is estimated to occur in 0.5% of pediatric cardiac necropsies.[1-5]
In most patients, CPVS can be repaired by open-heart angioplasty but percutaneous balloon catheter angioplasty may cause restenosis significantly. In surgical methods, living autologous atrial tissue repair and sutureless in situ pericardium repair have a better long-term result and a lower restenotic rate. They have been increasingly accepted but the traditional operation, artificial patch repair, was no longer employed in recent years because of its high rate of restenosis. Repair of CPVS with living autologous atrial tissue was reported first by Pacifico and his colleagues in 1984.[6] This method widens right pulmonary venous stenosis with a flap of interatrial septum and left pulmonary venous stenosis with left atrial appendage. Because of the growth potential of autologous atrial tissue, this method will provide lasting relief of obstruction. Sutureless in situ pericardium repair was reported first by Lacour-Gayet F and his colleagues[7] in 1995 to repair acquired right pulmonary venous obstruction after correction of total anomalous pulmonary venous connection (TAPVC) and was used in congenital right pulmonary venous stenosis in 2005.[8] Because of its "no-touch" technique, sutureless repair with in situ pericardium reduces the risk of subsequent restenosis. In our patient, living autologous atrial tissue repair and sutureless in situ pericardium repair were employed in combination to relieve bilateral pulmonary venous stenosis, and the short-term result was excellent.
Perfusion of the pulmonary artery with hypothermic protective solution during CPB was proved to be an effective method for lung protection, especially for patients with severe pulmonary hypertension.[9,10] The postoperative course of this patient was uneventful. Based on previous studies we believed that the result was at least partly associated with the employment of lung protection.
In short, CPVS is a rare malformation with very poor operative results. The child we report is the first patient who underwent a successful bilateral pulmonary venous angioplasty with living autologous atrial tissue repair combined with sutureless in situ pericardium repair in China.
Funding: None.
Ethical approval: Not needed.
Competing interest: None declared.
Contributors: LYL proposed the study and wrote the first draft. SXD analyzed the data. All authors contributed to the design and interpretation of the study and to further drafts. LJR is the guarantor.
References
1 Adey CK, Soto B, Shin MS. Congenital pulmonary vein stenosis: a radiology study. Radiology 1986;161:113-117.
2 Driscoll DJ, Hasslein PS, Mullins CE. Congenital stenosis of individual pulmonary veins: clinical spectrum and unsuccessful treatment by transvenous balloon dilatation. Am J Cardiol 1982;49:1767-1773.
3 Hyde JA, Stumper O, Barth MJ, Wright JG, Silove ED, de Giovanni, et al. Total anomalous pulmonary venous connection: outcome of surgical correction and management of recurrent venous obstruction. Eur J Cardiothorac Surg 1999;15:735-741.
4 Michielon G, Di Donato RM, Pasquini L, Giannico S, Brancaccio G, Mazzera E, et al. Total anomalous pulmonary venous connection: long-term appraisal with evolving technical solutions. Eur J Cardiothorac Surg 2002;22:184-191.
5 Ricci M, Elliott M, Cohen GA, Catalan G, Stark J, de Leval MR, et al. Management of pulmonary venous obstruction after correction of TAPVC: risk factors for adverse outcome. Eur J Cardiothorac Surg 2003;24:28-36.
6 Pacifico AD, Mandke NV, McGrath LB, Colvin EV, Bini RM, Bargeron LM Jr. Repair of congenital pulmonary venous stenosis with living autologous atrial tissue. J Thorac Cardiovasc Surg 1985;89:604-609.
7 Lacour-Gayet F, Zoghbi J, Serraf AE, Belli E, Piot D, Rey C, et al. Surgical management of progressive pulmonary venous obstruction after repair of total anomalous pulmonary venous connection. J Thorac Cardiovasc Surg 1999;117:679-687.
8 Yun TJ, Coles JG, Konstantinov IE, Al-Radi OO, Wald RM, Guerra V, et al. Conventional and sutureless techniques for management of the pulmonary veins: evolution of indications from postrepair pulmonary vein stenosis to primary pulmonary vein anomalies. J Thorac Cardiovasc Surg 2005;129:167-174.
9 Wei B, Liu Y, Wang Q, Yu C, Long C, Chang Y, et al. Lung perfusion with protective solution relieves lung injury in corrections of Tetralogy of Fallot. Ann Thorac Surg 2004;77: 918-924.
10 Liu Y, Wang Q, Zhu X, Liu D, Pan S, Ruan Y, et al. Pulmonary artery perfusion with protective solution reduces lung injury after cardiopulmonary bypass. Ann Thorac Surg 2000;69:1402-1407
Received May 15, 2006 Accepted after revision July 10, 2006
|

